Abstract
INTRODUCTION
The hypomethylating agents (HMAs), decitabine (DEC) and azacitidine (AZA), have made it possible to treat more elderly patients with acute myeloid leukemia (AML). Both HMAs have demonstrated efficacy in monotherapy and in combination with targeted therapies. However, there is little direct comparative data on AZA and DEC in first-line treatment, and we do not know which group of patients might benefit from each drug. Results of the full analysis set (FAS) were presented previously (Labrador J, et al. ASH 2020). Here, we report long-term clinical efficacy from prespecified patient subgroup analyses.
METHODS
We conducted a retrospective study to compare real-life clinical outcomes between AZA and DEC in patients with AML ineligible for intensive chemotherapy included in the PETHEMA registry, and analyzed clinical variables associated with response and overall survival (OS) between AZA and DEC.
RESULTS
A total of 626 patients were included for the FAS between 2006 and 2019. 487 (78%) received AZA and 139 (22%) received DEC. Baseline characteristics were comparable in both groups, except for the percentage of bone marrow blasts (44% vs. 34% in the DEC group compared to AZA, p=0.010).
In the FAS, there was no difference in the CR, CR/CRi or ORR (CR/RCi + PR) rate: 18%, 20.5% and 32% with AZA vs. 23%, 25% and 39.5% with DEC (p=0.20, p=0.27 and p=0.12).
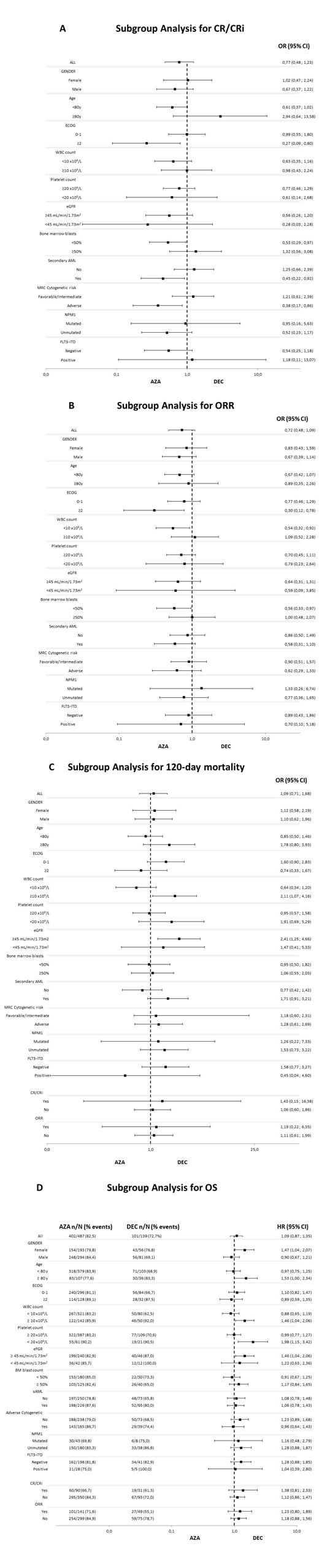
In the subgroup analysis, DEC was associated with higher CR/CRi rate than AZA in patients with ECOG ≥ 2 (95% CI: 0.088 - 0.801), bone marrow blast count < 50% (95% CI: 0.293 - 0.965), secondary AML (95% CI: 0.223 - 0.918) and adverse cytogenetics (95% CI: 0.171 - 0.857) (Figure 1A). DEC was associated with higher ORR rate than AZA in patients with ECOG ≥ 2 (95% CI: 0.116 - 0.782), leukocytes < 10 x10 9/L (95% CI: 0.321 - 0.920) and bone marrow blasts < 50% (95% CI: 0.321 - 0.920) (Figure 1B)
120 days-mortality was 25.4% after AZA and 27.1% after DEC, p=0.70. Patients who did not achieve at least a PR had significantly higher 120-day mortality with both HMAs (OR 8.85 and 8.22 for AZA and DEC, respectively). In the subgroup analysis, patients with leukocytes ≥ 10 x10 9/L (95% CI: 1.069 - 4.157) and those with estimated glomerular filtration rate (eGFR) ≥ 45 mL/min/1.73m 2 (95% CI: 1.249 - 4.664) had higher 120-day mortality with DEC than with AZA (Figure 1C)
With a median follow-up of 12 months, median OS was 10.4 months (95% CI: 9.2 - 11.7) for AZA vs. 8.8 months (95% CI: 6.7 - 11.0) for DEC (p = 0.455). The subgroup analysis revealed that patients ≥ 80 years (95%: CI 1.005 - 2.341), with leukocytes ≥ 10 x10 9/L (95% CI 1.039 - 2.062), platelet count <20 x10 9/L (95% CI: 1.150 - 3.422) and those with eGFR ≥ 45 mL/min/1.73m 2 (95% CI: 1.040 - 2.059) did benefit for treatment with AZA compared to DEC (Figure 1D).
CONCLUSIONS
Our study provides real-life data on the outcomes of AML patients treated with AZA compared to DEC in a large retrospective cohort with long-term follow-up. In addition, we identify for the first time some baseline characteristics that could benefit from AZA or DEC in terms of responses, 120-day mortality and OS. These findings could help us to choose the most appropriate HMA in monotherapy or for the development of new combinations.
de la Fuente: Novartis: Research Funding; Abbie: Consultancy, Speakers Bureau; Incyte: Consultancy, Speakers Bureau; BMS: Consultancy, Speakers Bureau. Tormo: Novartis: Consultancy, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Jazz Pharmaceuticals: Consultancy, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Pfizer: Consultancy, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Amgen: Consultancy, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Astellas: Consultancy, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau. Pérez-Simón: Novartis: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau. Montesinos: Forma Therapeutics: Consultancy; Tolero Pharmaceutical: Consultancy; Karyopharm: Membership on an entity's Board of Directors or advisory committees, Research Funding; Novartis: Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Pfizer: Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Sanofi: Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Janssen: Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Incyte: Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Daiichi Sankyo: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Celgene: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Glycomimetics: Consultancy; Agios: Consultancy; Stemline/Menarini: Consultancy; Teva: Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; AbbVie: Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Astellas Pharma, Inc.: Consultancy, Honoraria, Other: Advisory board, Research Funding, Speakers Bureau.
Author notes
 This icon denotes a clinically relevant abstract
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal